
The Health Effects of Histamine Sensitivity and Intolerance
TL;DR: Histamine Sensitivity
- Some people can’t break down histamine effectively due to low DAO enzyme activity, leading to buildup in the body.
- Trigger foods include red wine, citrus, chocolate, fermented foods, aged meats/cheese, leftovers, and certain additives.
- Symptoms occur when your “histamine bucket” fills up and overflows from accumulated exposure.
- Hormones (especially estrogen) and gut health can significantly impact histamine levels.
Issue #7 - Histamine Sensitivity and Intolerance
Have you ever felt like red wine just doesn't agree with you? Do you feel bad after drinking orange juice? How about certain cheeses or even chocolate?
I might have some leads for you.
Histamine sensitivity or intolerance has been fairly recently identified as a condition that approximately 1% of the population is affected by.
This condition can negatively impact your life in a big way. Our bodies make histamine, but people are quite often surprised to learn that it also comes from outside sources such as food or medications.
Basically, some people, like myself, aren't as effective at breaking down histamine that comes from the food we eat or medications we take. This issue results in a long list of symptoms that you might be shocked to discover are symptoms you experience. But, this 1% isn't the 1% you want to be in.
Let's cut to the case. You want to know what symptoms I am talking about.
Here are but a few:
And if you want to know what types of food I am talking about, here are a few:
What is histamine anyway?
It's a signaling chemical your immune system makes as part of your body's defense system. It protects us. Although it is involved in many functions, including sleep regulation, cognition and digestion, histamine plays a key role in your body's inflammatory response.
There are four different types of receptors found in your cells that histamine attaches itself to. Which receptor it attaches to will determine the type of symptom you can get.
The main two receptors for the purpose of this article are H1R and H2R.
The H1R receptors are found throughout your body, including the smooth muscle cells of your airways and blood vessels. When these receptors are triggered you get symptoms like sneezing, runny nose, itchy eyes and swelling of airways.
The H2R receptors are mainly found in your stomach cells that release acid, smooth muscle cells and heart cells. When these receptors are triggered you get symptoms like heartburn (secretion of stomach acid), headaches and tachycardia.
Is histamine sensitivity/intolerance the same as an allergic reaction?
No, this is completely different from an allergic reaction. An allergic reaction is an immune system response. A food allergy is a reaction of the immune system where immunoglobulin E (IgE) anti-bodies are produced and inflammatory mediators like histamine, which regulates inflammation, are released very quickly.
This sensitivity is a deficiency in how a person processes histamine that has come from food.
We produce an enzyme called diamine oxidase (DAO) that breaks down histamine coming from food. When DAO isn't doing its job properly, you have too much histamine in your body and symptoms can appear. A second enzyme called HNMT plays less of a role so I won't be going into detail on this one.

If you are low in DAO, you have less DAO to put to work when you ingest high histamine foods.
Our genetic make-up affects how much DAO we produce. I have had my DNA tested and I discovered that more than one DAO enzymatic pathway is deficient or weak. So, when I eat something high in histamine potential, I have less of the enzyme to deal with it.
In addition, we all have different amounts of histamine that we can tolerate in the first place.
Imagine that you have a bucket and that bucket contains the amount of histamine your body can easily break down. If it overflows, you have too much histamine floating around in your body. Now, your bucket could also be bigger than mine so the amount of histamine you can handle is more than me.
When you combine a smaller histamine bucket with less DAO enzymes, you have a recipe for histamine sensitivity.
In other words, we could both eat the same diet everyday and I could have symptoms of too much histamine whereas you are just fine.
It can take time to fill your bucket so it is the accumulation of histamine from all the food you eat that triggers the problem.
This gets tricky when you are trying to identify the culprit and why recording what you eat helps you figure out what is contributing to filling your bucket. If you eat sauerkraut everyday, you fill the bucket a lot faster than if you eat sauerkraut once a week.
To complicate matters even more, histamine is connected to estrogen.
Hormonal changes that occur during pregnancy or menopause can make symptoms a lot better or a lot worse. During pregnancy, the placenta makes a lot of DAO to protect the fetus and, as a result, some women find their histamine sensitivity symptoms disappear completely.
Peri-menopause and menopause are a whole different story as they can cause symptoms to worsen or even appear for the first time.
To simplify things, imagine a vicious circle where spikes in estrogen increase histamine which then turns around and increases estrogen. Round and round it goes while you deal with heartburn, hives and headaches. Your DAO enzymes are depleted and can't keep up with the merry-go-round from hell.
How is histamine formed in food?
In meat, the amino acid histidine turns into histamine after it's been cooked. The longer the amount of time between cooking and eating, the higher amount of histamine. That's why leftovers are a problem for people with histamine sensitivity.
It's recommended that you freeze your meat leftovers to stop the increase in histamine as it will still increase in the fridge, but at a slower pace than at room temperature.
It's also why bone broth, which has been stewing at low heat for hours and hours, is loaded with histamine.
If bone broth doesn't agree with you, this issue could be why.
Fermented foods contain histamine as a result of yeast and bacteria converting histidine into histamine during the fermentation process. Fermented vegetables will have less histamine than fermented foods higher in protein like yogurt because protein provides more histidine to work with.
Some foods have high histamine, some liberate histamine from your body and some block your DAO enzyme.
For the purpose of this article, I provided a list of foods to be aware of rather than going into too much detail about which category they belong to. This isn't an exhaustive list, but rather a summary of common foods. Check out the link to a large list of foods I have below or even a do a quick internet search that includes the name of the food and the word “histamine” to get more information.
Let's look at our gut microbiome and probiotics.
There are types of bacteria in our gut that produce an enzyme that converts histidine from protein into histamine. When you have a lot of these types of bacteria, the histamine level in your digestive tract will be higher. Some strains of probiotics are histamine producers so its worth doing some research if you are concerned about your probiotic brand.
There are also types of bacteria in our gut that produce DAO and can then help break down histamine for us.
Does that mean you can just buy a probiotic and the problem is solved? That hasn't been my experience. I have tried a variety of probiotics claiming to be low histamine or high DAO, but they didn't make a difference for me. That said, you could find they make a difference for you as everyone's gut is different.
Let's get to some encouraging information. There are things you can do to manage your histamine level.
Thankfully, there is a lot of information online these days to help you figure out what to eat and how to support your body's ability to produce DAO.
What are the chances your family physician is going to know what you are talking about when you bring this up? Not high. Alternative health professionals like naturopaths or those in functional medicine are more likely to be knowledgeable.
My main source of information for this article is Histamine Intolerance: The Comprehensive Guide for Healthcare Professionals by Dr. Janice Joneja. Dr. Joneja's book helped me understand what was happening to me and what I could do about it.
This list from the Swiss Interest Group Histamine Intolerance (SIGHI) has been my go-to for checking the histamine potential for all kinds of foods, additives, spices, etc. for many years.
If you have done any DNA testing through Ancestry.com or 23andMe or SelfDecode, you can use that data to buy the report ($95) I used to get my answers. You just upload your data and they generate a report that analyzes different enzyme pathways, including histamine, and explains how your health could be affected and gives you suggestions for improving the function of those pathways.

This report, called Stratagene, has helped me tremendously. It's given me answers I couldn't find any other way (trust me, I looked) and helped me understand why I experienced symptoms I couldn't explain.
Dr. Ben Lynch from Seeking Health now has a report specifically covering histamine as well. I bought the main Stratagene report which covers many different enzymatic pathways, so I can't comment on the contents of his new report.
Can you help your body make more DAO? Yes, you can. Magnesium, vitamin C, vitamin B6, zinc and copper are all involved in supporting your DAO enzymatic pathways.
You can also take DAO supplements, which are normally sourced from the kidneys of pigs.
I take them everyday, at least once a day, depending on what I am eating. I take DAO from Seeking Health because it has less inactive ingredients in it and it's a great price compared to other brands. Other brands contain titanium dioxide which caused side effects for me. I will write about inactive ingredients like titanium dioxide in a future article.
I'll bet you are thinking to yourself, why doesn't she just take an anti-histamine?
Well, here's why it's not a long term solution.
Anti-histamines like Benedryl, Claritin or Zyrtec don't break down histamine or stop histamine from being released in the first place; they block histamine from attaching to your cell's H1R receptors.
So, you can get some temporary relief, but as soon as the anti-histamine wears off, the receptors are no longer blocked and the histamine that has been floating around waiting for its opportunity to latch on to the receptor does just that.
Next thing you are asking is, what about antacids or heartburn medications?
Can they help? Antacids will neutralize the acid in your stomach so they can stop a flareup of gastric symptoms but they can't block histamine or stop it from being released.
Medications like Tagamet, Zantac or Pepcid, are designed to reduce symptoms of acid reflex or heartburn by blocking histamine from attaching to the H2R receptors in your stomach so less acid is produced. They aren't a long term solution because you don't want to lower your stomach acid level continuously.
Heartburn medications like Nexium are proton pump inhibitors (PPI's) that stop stomach acid from being pumped into the stomach. They don't block histamine from attaching to the H2R receptors or stop histamine from being released. They can help with a flareup as well but doctors don't recommend them for long term use.
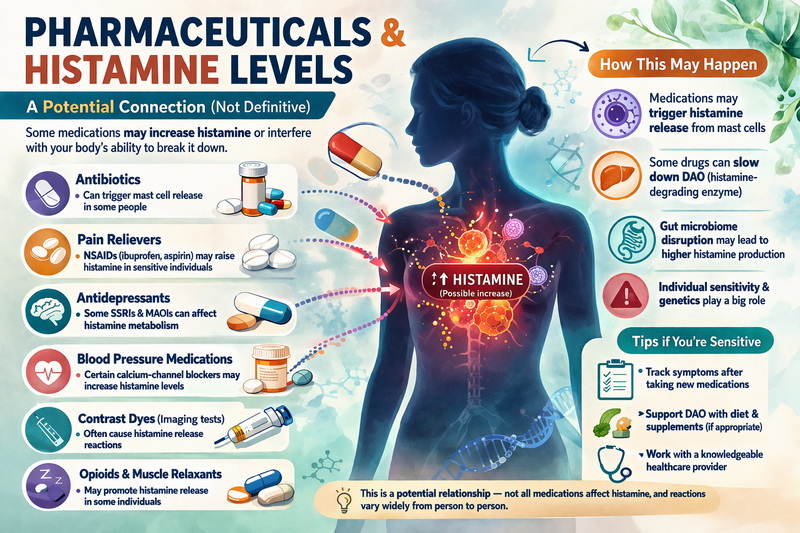
Like foods, pharmaceuticals affect histamine levels by either increasing its release and/or blocking DAO activity.
I mention the following medications not to cause you to worry or think you have to stop taking them, but so you can consider how you feel if and when you take them especially if you think you may have issues with histamine. This information might help explain side effects or a past experience you had with a medication.
NSAIDS (non steroid anti-inflammatory drugs) like Aleve and Advil have the ability to block DAO as well as cause mast cells to release more histamine. Metformin, some antibiotics and some anti-depressants like Citalopram can also block the DAO enzyme.
Other drugs have the ability to stimulate the release of histamine. Drugs like opioids, anesthetics, beta blockers and the contrast dyes used in MRI and CT scans are included in this category.
I experience many of the symptoms listed above, but my main symptoms are heartburn and swelling in my throat. Thankfully, they don't normally happen together.
For example, fermented foods will trigger heartburn (H2R receptor) whereas citrus and other fruits will cause my throat to swell (H1R receptor).
I first experienced my throat swelling up (not enough to stop breathing, but enough to scare the heck out of me) when I was in my 20's, about 30 years ago. With my limited knowledge at the time, I had narrowed the problem down to eating strawberries. At that time, not much was known about histamine sensitivity so the allergy specialist my doctor referred me to had no clue what was happening to me.
My experience wasn't matching the allergy testing he did. Remember that allergies are not the same thing so testing for IgE anti-bodies wasn't going to explain this symptom. Rather than digging further, he sent me on my way, telling me it was all in my head. Funny thing was that he said it in such a nice way that I didn't realize I had been insulted until I was in the parking lot.
When my histamine bucket overflows, it can take days and sometimes weeks to calm down. I have had flareups that required 48 hour fasting and then eating only plain oatmeal in between sodium bicarbonate/potassium bicarbonate antacid drinks to resolve.
Food hasn't been my only problem as I have had reactions to medications as well.
I was prescribed Imovane (Zopiclone), a sleeping pill, by a specialist to see if improving my sleep would help with some of my fatigue related symptoms. After a few weeks, I was getting heartburn everyday, no matter what I ate. I was in tremendous pain and miserable.
When I brought up the possibility of the medication being the culprit because I could not pinpoint any other cause, the specialist flat out told me it was IMPOSSIBLE.
A few more weeks go by and I am experiencing raging heartburn everyday that nothing is helping and I'm afraid of burning a hole in my throat. I took matters into my own hands and stopped taking the medication. One day later the heartburn was gone. When I told the specialist how the heartburn had resolved when I stopped the medication, she said nothing and moved on to another subject.
Here's the message: doctors don't always have all the answers.
I had been prescribed Propranolol, the beta blocker, for my “inappropriate” tachycardia by a cardiologist. Just minutes after taking the medication, my throat started to swell up at a speed I hadn't felt before. I didn't know if it was histamine related and would plateau and then calm down or if it was an allergic reaction that could have been deadly. Off I went to the nearby ER. Luckily, it turned out to be histamine related and things calmed down.
My most recent medication related histamine adventure occurred when I tried CBD oil for pain relief.
The CBD, in a coconut oil base, caused heartburn with just one drop. So, I tried holding the oil under my tongue for 5 minutes to absorb the CBD and then spit it out. No heartburn. Now, after a few weeks of increasing the number of drops and still spitting it out, I woke up one morning to discover Stewie from Family Guy starring back at me in the mirror. My face had swollen up like a balloon!
Since I hadn't ever experienced any histamine issues with coconut oil, the base oil for the product, the prescribing doctor determined it was something in the CBD that triggered the reaction. No more CBD for me. And, it was the one time I experienced both receptors going crazy from the same ingredient.
Managing histamine sensitivity is a daily concern for me.
I watch what I eat and avoid the foods that I know will quickly cause a reaction. I take DAO supplements with meals that include leftover meat and other high histamine foods. I also support my DAO pathways with vitamins and minerals. I am continuing to work on balancing my gut microbiome and will write about it in a future article.
When I feel a flareup starting I take more DAO to calm things down. I also drink plenty of water and make sure I eat only low histamine foods for the next couple of days.
If heartburn is the problem and it doesn't improve within a day or two, I have to try a sodium bicarbonate/potassium bicarbonate drink recommended by Dr. Joneja.
Mix together:
2 tablespoons sodium bicarbonate (baking soda)
1 tablespoon potassium bicarbonate (sold as a supplement and for non-medical purposes)
For one dose, mix ½ teaspoon of the mixture in ½ cup water water and drink. You can do it again in twenty minutes if the first dose doesn't help. But, wait 24 hours if you have to try it again.
Every new supplement I consider taking is researched to see if there is any data regarding its histamine potential.
Many promising supplements have been ruled out because of their potential for triggering a histamine problem.
If you experience a side effect from eating any of the foods listed above, perhaps it is worth investigating the possibility your histamine bucket is overflowing and your DAO enzyme pathway needs some support.
Stay tuned for the next issue of Good Health...Under Construction where I write about weighted blankets.
Nick's sister, Alexis
More From Fitstep.com
| Stink Training for Bringing Up Weak Bodyparts | |
| Fat Loss Circuit Training With Dumbbell Crawling | |
| The Great Big List of Calorie-Free Foods | |
| 4 Tips For Larger, Firmer, Rounder Glutes |
Site Search
Subscribe to my YouTube Channel
And see every new exercise and training technique when it's released!
Recommended For You...
The Starting Monday Diet
Learn how to eat for fat loss WITHOUT losing muscle or strength. This simple, week-based diet program will get you ripped AND strong. This is the best "no guilt" diet program I've ever put together.
Discover the easiest way to get lean and KEEP your muscle...



